We often say that a picture is worth a 1,000 words. In podiatry, x-rays are like a picture and they, too, are worth 1,000 words. In this case example, the patient suffered from a bunion deformity (hallux valgus) shown in X-ray #1 taken with the patient standing and the x-ray camera looking down:
X-ray #1
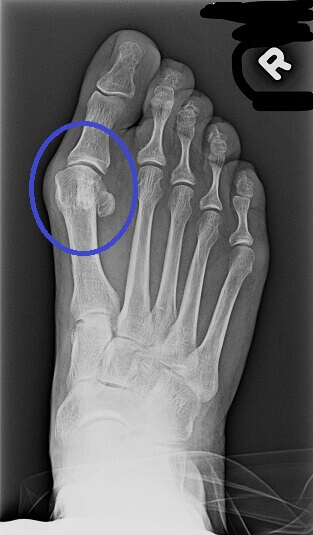
This is called an AP (anterior-posterior) view or DP (dorso-plantar) view. Standard foot x-rays, when taken for surgical planning for bunion surgery, should always be taken in full weight bearing so that the surgeon can determine the splay of the foot. The relationship of some of the important bones in bunion surgery can change when going from no weight bearing to full weight bearing.
The circle is around the metatarso-phalangeal joint. The great toe is angled toward the second toe and slightly overlapping it. The goal of most bunion correction surgeries is to move the head of the first metatarsal toward the second metatarsal. There are many procedures that accomplish this. In some, the entire metatarsal is re-positioned and fused to the cuneiform (bone). In other procedures, the metatarsal is cut with the 2 parts re-positioned, then held in place with absorbable or metallic screws.
In the surgery performed on this patient, the surgeon chose to cut the metatarsal and re align it. X-ray #2 is post-operative and shows the result of the surgery:
X-ray #2
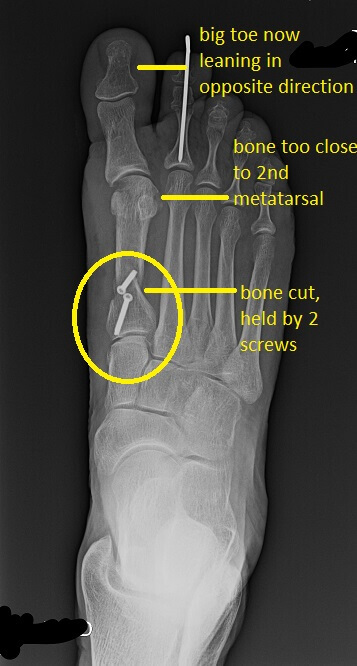
Starting at the bottom of the x-ray, the metatarsal was cut with a bone saw and held in position with 2 screws. However, the surgeon miscalculated and moved the bone too far over. The bone (the 1st metatarsal) is now too close to the 2nd metatarsal.
Foot surgeons use a variety of measurements when evaluating x-rays in order to determine how much the bones are deformed and therefore how much the bones need to be re-aligned. In this example, the key measurement is known as the intermetatarsal angle. This is the angle formed by a straight line draw along the long axis of the 1st metatarsal and a similar line drawn through the 2nd metatarsal. The angle formed is known as the “intermetatarsal angle.” The normal intermetatarsal angle is between 0-8 degrees. In this example, the pre-operative intermetatarsal angle was greater than 8 degrees. The surgeon made the intermetatarsal beyond 0 degrees or into a “negative” intermetatarsal angle. This is considered malpractice. The angle should not be less than 0 degrees.
If the angle is less than 0 degrees it is likely that the great toe will move in the opposite direction. That direction is known as “hallux varus.” In X-ray #2 the great toe is in the position of “hallux varus.” Proper foot function is often ruined if the great toe is not properly positioned. Some patients can function with a hallux varus if they can tolerate the embarrassment from an oddly deformed-looking foot, and if they can squeeze the great toe into a shoe and comfortably walk. Most cannot.
When a surgeon sees that she miscalculated and created a hallux varus, it is incumbent upon the surgeon to do something to stop the big toe from moving further away from the 2nd toe. Sometimes a brace suffices but more often surgery is needed to get the bones into their correct position. In this case, the surgeon failed to realize that surgery was needed. The patient continuously complained of more pain than he had before surgery because of the hallux varus, and of his inability to properly fit into a shoe, and walk comfortably.
X-ray #3 shows a worsening of the hallux varus:
X-ray #3
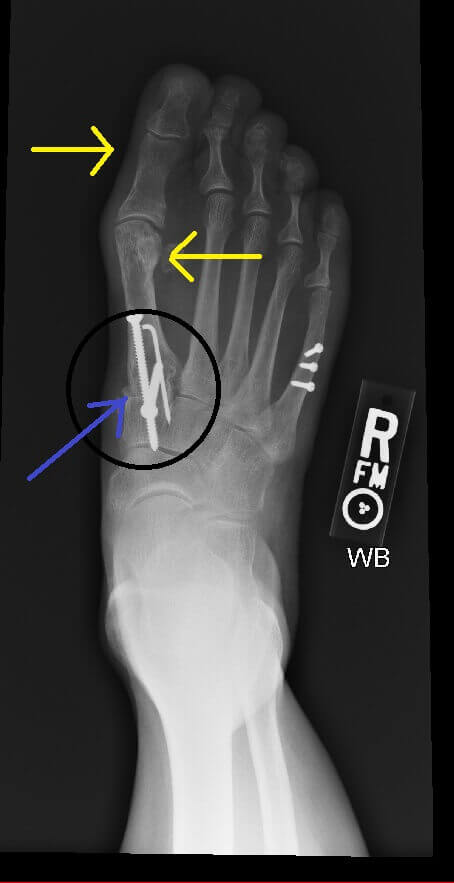
The patient went to another foot surgeon who performed 2 surgeries to get the foot properly working again. We will discuss those in another blog.

